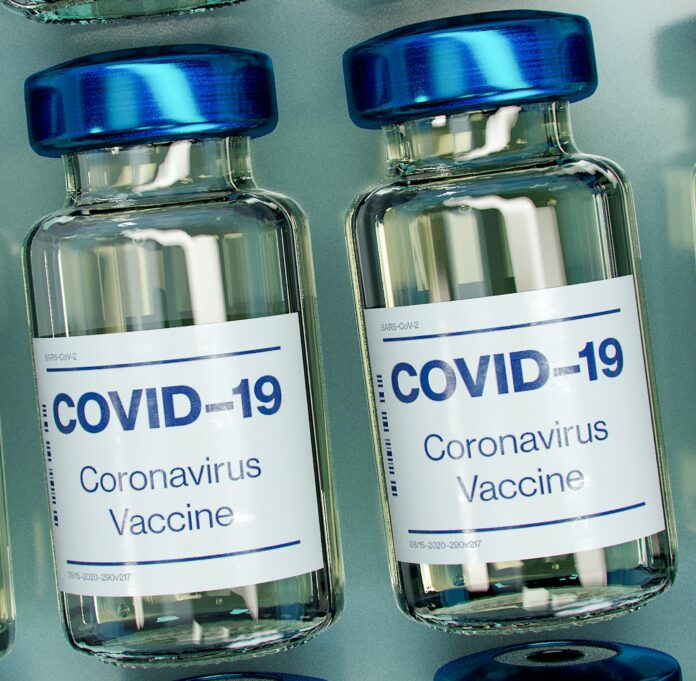
As older teens and young adults become eligible for COVID-19 vaccination across the country, and younger teens await their turn, new survey data suggest a strong readiness that has grown since fall. But just as with older generations, a shrinking but still sizable minority of people age 14 to 24 say they’re not willing to get vaccinated, or that their decision will depend on safety.
That makes it crucial for public health authorities, health care providers and others to create vaccination-related materials that reach young people in ways that are relevant to them. The data, from the text-message-based MyVoice national survey of youth based at the University of Michigan, are published in a new paper in the Journal of Adolescent Health, and supplemented by new polling data just received in the past week.
Eric Brandt, M.D., M.H.S., lead author of the new paper, notes that in the first MyVoice survey in October 2020, 76% of the 911 teens and young adults said they were willing to get vaccinated, though that included 33% who said their ultimate decision would depend on additional information. At that time, 20% of young people said they were unwilling to get a COVID-19 vaccine. Brandt’s colleague Stephen Gorga, M.D., has just finished analyzing data from MyVoice respondents who answered a repeat survey in late March 2021.
The percentage who say they’re willing to get vaccinated, or already have been vaccinated, has risen to 84%. Nine percent of the total say they’re willing but that their decision still depends on what they learn about the vaccine. That means that 75% are unconditionally willing to get the vaccine when it becomes available to them, or already have been vaccinated. The percentage of people age 14 to 24 who say they are not willing or intending to get vaccinated is down to 15%.
“These data reassure us that most youth are willing to get vaccinated against COVID-19 if they feel the vaccine is safe and effective,” says Brandt. “But concerns about vaccine safety are still very much alive in this group.”
He notes that the newest data were gathered before the U.S. Food and Drug Administration announced its “pause” of use of the Johnson & Johnson/Janssen vaccine due to a small number of cases of a rare blood clot condition in younger women who were among the first 6.7 million Americans to get the vaccine. The Astra-Zeneca vaccine, which is not available in the United States, has been paused in some countries because of clot concerns, too.
Currently, the Pfizer/BioNTech vaccine has emergency approval for use in Americans age 16 and up, while the Moderna and J&J vaccines have such approval for people age 18 and up. The new MyVoice data were also gathered before Pfizer announced results from its study of its vaccine in people age 12 to 15, and its intention to see approval in this age group soon. Moderna has also just announced that enrollment in its clinical trial for ages 12 to 17 has been completed.
Other findings
In the new paper, Brandt and colleagues – including MyVoice director Tammy Chang, M.D., M.P.H., M.S., share other findings from the October poll.
At that time, Black young people were more than three times more likely than their white peers to say they weren’t willing to get the vaccine when it became available. Meanwhile, young people of Asian descent were more likely than white or Black young people to say they’d get vaccinated.
As communications efforts shift to younger people, the study finds that organizations such as the Centers for Disease Control and Prevention, and the World Health Organization, are the preferred sources of vaccine information for 42% of young people, and that 32% said they would prefer to learn about the vaccine from a health professional such as a doctor, pharmacist or other provider or health care organization.
Among those who said in October that they weren’t willing to get the vaccine, safety was the top concern, especially what some saw as an inadequate amount of time in testing. Only 2% mentioned conspiracy theories. The role of younger people in spreading COVID-19, even if they generally have a lower risk of developing severe disease, makes it important to reach them with effective messages and transparent information and answers to their questions, Brandt says.
Special efforts to reach Black teens and young adults may be needed, because of the disproportionate risk they and their family members face. Otherwise, racial disparities already well-documented in COVID-19 outcomes may continue to increase.
Brandt, Gorga and Chang are all members of the U-M Institute for Healthcare Policy and Innovation. Brandt is a cardiologist at the U-M Frankel Cardiovascular Center; Gorga is a pediatrician at C.S. Mott Children’s Hospital and Chang is a physician in the Department of Family Medicine.
Story Credit: Newswise
Photo Credit: Daniel Schludi/Unsplash