(Family Features) Diagnosing a transient ischemic attack (TIA), sometimes called a “warning stroke,” can be challenging because symptoms often disappear within an hour. However, it’s important to seek emergency assessment to help prevent a full-blown stroke.
While a TIA, which is a temporary blockage of blood flow to the brain, doesn’t cause permanent damage, nearly 1 in 5 people who have a suspected TIA will have a stroke within three months, according to a scientific statement published in the American Heart Association journal “Stroke.” Additionally, almost half will occur within two days – which is why TIAs are often described as warning strokes.
People with cardiovascular risk factors, such as high blood pressure, diabetes, obesity, high cholesterol and smoking, are at high risk for stroke and TIA. Other conditions that increase risk include peripheral artery disease, atrial fibrillation, obstructive sleep apnea and coronary artery disease. In addition, a person who has had a prior stroke is at high risk for TIA.
TIA symptoms are the same as stroke symptoms, only temporary. They begin suddenly and may have any or all these characteristics:
* Symptoms begin strong then fade
* Symptoms typically last less than an hour
* Facial droop
* Weakness or numbness on one side of the body
* Trouble finding the right words or slurred speech
* Dizziness, vision loss or trouble walking
The F.A.S.T. acronym for stroke symptoms can also be used to identify a TIA: F – face drooping or numbness; A – arm weakness; S – speech difficulty; T – time to call 9-1-1, even if the symptoms go away.
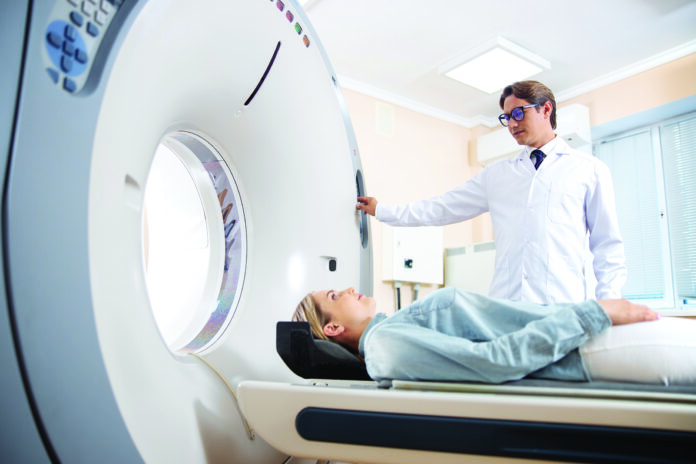
Given the appropriate scan, 2 in 5 people will learn they actually had a stroke rather than a TIA, according to the scientific statement, which highlights the importance of seeking prompt medical attention. Upon arrival to the emergency room, a series of tests may be completed after assessing symptoms and medical history, including a CT scan, MRI and blood tests.
* CT Scan – a non-contrast scan used to look at the blood vessels in the head and neck to rule out brain bleeding and TIA mimics (conditions that share some signs with TIAs but are due to other medical conditions such as low blood sugar, seizure or migraine). A CT scan may also be used to assess the neck arteries; nearly half of people with TIA symptoms have narrowing of the large arteries leading to the brain.
* MRI – The preferred way to rule out a brain injury, such as a stroke, magnetic resonance imaging (MRI) is typically done within 24 hours of symptoms beginning. Because some emergency rooms may not have access to an MRI scanner, patients may be admitted to the hospital or transferred to a center. About 40% of patients who go to the emergency room with TIA symptoms are diagnosed with a stroke based on MRI results.
* Blood Tests – Blood work will typically be completed to rule out conditions that may cause TIA-like symptoms, such as low blood sugar or infection, and check for cardiovascular risk factors like diabetes and high cholesterol.
Once a TIA is diagnosed, a cardiac checkup should be completed within a week of having a TIA, if not done in the emergency room. Consultation with a neurologist should also be completed within 48 hours (no longer than one week) after experiencing a TIA, as early consultation with a brain specialist is associated with lower death rates after a TIA.
To learn more and find additional resources, visit Stroke.org.
Photo courtesy of Getty Images
#16782
Source: American Heart Association